Vicodin
Learn More About Vicodin
How Does Vicodin Work?
Vicodin is a combination of hydrocodone and acetaminophen. Hydrocodone is a semisynthetic opioid that binds to the brain’s mu-opioid receptors, blocking pain signals. This binding also triggers the release of dopamine, which can create feelings of euphoria, making Vicodin potentially addictive. Acetaminophen works as a non-opioid pain reliever, enhancing the overall analgesic effect of hydrocodone. This dual action makes Vicodin effective for pain relief but also increases its risk of addiction and overdose.
What are the Different Forms of Vicodin?
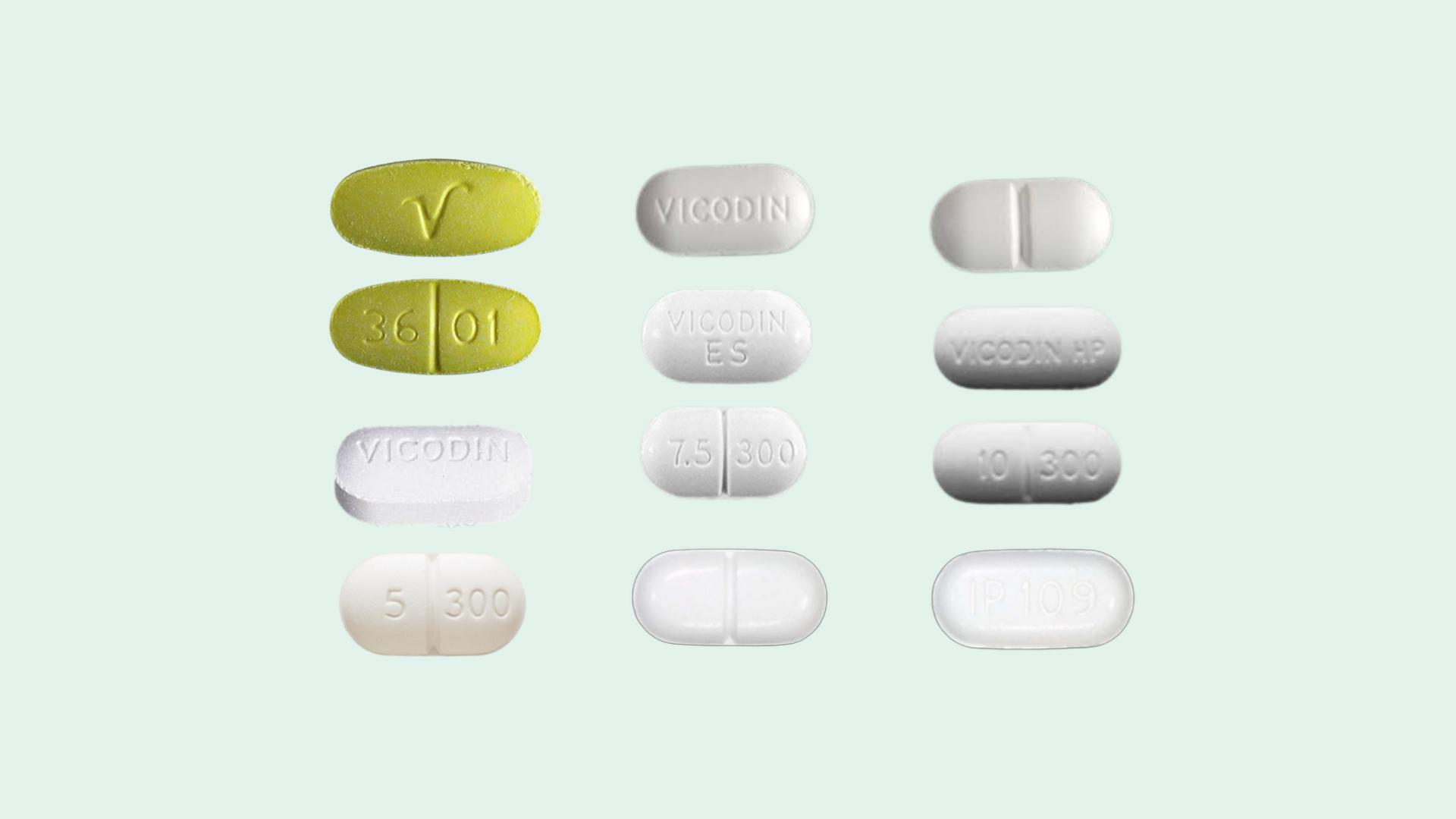
Vicodin is available in several formulations, primarily varying in the ratio of hydrocodone to acetaminophen. Traditional Vicodin formulations include
- Vicodin 5/300: 5 mg hydrocodone and 300 mg acetaminophen
- Vicodin ES: 7.5 mg hydrocodone and 300 mg acetaminophen
- Vicodin HP: 10 mg hydrocodone and 300 mg acetaminophen
Other brands, like Norco, offer similar combinations but with different acetaminophen ratios, which can affect both efficacy and side effects. Extended-release formulations are also available for chronic pain management, allowing for less frequent dosing but requiring careful patient monitoring due to higher abuse potential.
What is the Chemical Composition of Vicodin?
The active ingredient in Vicodin, hydrocodone, has a complex chemical structure: 4,5α-epoxy-3-methoxy-17-methylmorphinan-6-one tartrate (1:1) hydrate. It is derived from codeine and thebaine, which are natural alkaloids from the opium poppy. Acetaminophen, the other component, is a non-opiate analgesic with the chemical formula C8H9NO2. The combination of these two components allows for effective pain relief while also posing risks for hepatotoxicity, especially at high doses.
What Are the Medical Uses of Vicodin?
Vicodin is primarily prescribed for the management of acute pain following surgery or injury, as well as chronic pain conditions where non-opioid medications are ineffective. Clinical guidelines recommend using opioids like Vicodin only when safer alternatives have failed, reflecting a cautious approach to opioid prescribing. The Centers for Disease Control and Prevention (CDC) emphasizes the need for careful assessment of pain management strategies to minimize the risk of addiction and misuse.
What Are the Risks and Precautions for Vicodin Use?
Despite its effectiveness, Vicodin carries significant risks. The potential for Vicodin addiction is high, especially among individuals with a history of substance use disorders or those with co-occurring mental health conditions. The CDC reported that approximately 3.6 million Americans aged 12 and older misused hydrocodone in the past year, highlighting the scope of the problem.
Patients using Vicodin should be monitored closely for signs of misuse, particularly if they have risk factors such as a history of addiction, mental health disorders, or concurrent use of other central nervous system depressants like benzodiazepines or alcohol.
What Are the Side Effects of Vicodin?
Common side effects of Vicodin include
- Nausea
- Dizziness
- Drowsiness
- Constipation
- Dry mouth
More severe side effects can occur, particularly with long-term use or overdose, including respiratory depression, which can be life-threatening. Understanding these side effects is crucial for anyone using Vicodin, as they can significantly impact daily functioning and quality of life.
How Does Vicodin Impact Organ Systems?
Abusing Vicodin poses significant risks to overall health. Acute overdose can dangerously slow breathing, potentially leading to death. With prolonged use, the liver and kidneys—organs crucial for drug metabolism and elimination—may suffer considerable harm. The heart is not immune either; Vicodin abuse can trigger arrhythmias and increase susceptibility to various cardiac issues.
Which Are Signs of Vicodin Addiction?
Recognizing the signs of Vicodin addiction is vital for early intervention. Common indicators include:
- Taking more Vicodin than prescribed
- Engaging in “doctor shopping” to obtain multiple prescriptions
- Continuing use despite negative consequences, such as relationship or job issues
- Experiencing cravings or withdrawal symptoms when not using Vicodin
If you or someone you know is displaying these behaviors, it may be time to seek help.
How to Get Help for a Vicodin Addiction
The journey to recovery from Vicodin addiction often begins with acknowledging the problem. Various Vicodin treatment options are available, including:
Medical Detox
Supervised withdrawal management can help alleviate withdrawal symptoms and reduce cravings. This process typically lasts 10 to 20 days, with the most intense symptoms occurring in the first few days.
Medication-Assisted Treatment (MAT)
This approach combines medications like buprenorphine or methadone with counseling and behavioral therapies to address both the physical and psychological aspects of addiction.
Behavioral Therapies
Cognitive behavioral therapy (CBT) and other therapeutic modalities can help individuals develop coping strategies and address underlying mental health issues.
Inpatient vs. Outpatient Rehab
Depending on the severity of the addiction, individuals may benefit from inpatient treatment, which offers 24/7 support, or outpatient programs that allow for more flexibility.